Coronary artery calcification and… beyond calcification
In a previous blog post, we discussed the measurement of coronary artery calcification (CAC), a key indicator of heart disease risk. We also presented the results of our algorithm designed to automate this process. However, we do not want to focus here on technological far-fetched experiments.
AI-powered medical software manufacturers often talk about how their apps save doctors time and make diagnosis easier. But can we actually measure the real benefits for the whole society? Could they be measured when it comes to calcium score examination and the algorithm?

Can AI become a lifesaver?
We recently came across a clinical trial that we also shared on our LinkedIn profile [1]. This study is especially exciting because it’s the first of its kind to explore whether medical algorithm can help reduce number of… deaths. This was supposed to be the primary endpoint of the trial. Among myriads of AI clinical trials, it was quite a unique objective.
Researchers at Taiwan’s National Defense Medical Center conducted a large clinical trial “Applying an Artificial Intelligence-Enabled Electrocardiographic System for Reducing Mortality”. The study involved nearly 16,000 patients from multiple facilities. Researchers achieved a major win: using AI alerts on ECGs led to a noticeable decrease in the number of deaths within 90 days [2].
However, we don’t know the specifics of how the AI system influenced doctors’ decisions. In other words, we don’t know exactly how the AI prompted them to intervene or adjust treatment plans.
Coronary artery calcification as an independent predictor
The coronary artery calcification score (CAC score) emerged in the 1990s as a way to assess heart disease risk. Based on a heart CT scan we can detect calcium buildup in arteries. A higher score indicates a greater chance of future heart problems, atherosclerosis and coronary stenosis.
On the one hand, finding no calcification is a strong indicator that atherosclerosis isn’t present. However, the role of the CAC score in people with stable chest pain remains less certain. Or should I say: its role remained uncertain until recently.
Patients with stable chest pain benefits: a clinical study
Led by Dr. Marc Dewey, a radiology professor and vice chair at Charité, a team investigated the ability of coronary artery calcium score to predict major heart problems in 1,749 people (average age 60). These participants came from the DISCHARGE (Diagnostic Imaging Strategies for Patients with Stable Chest Pain and Intermediate Risk of Coronary Artery Disease) trial [3].
On March 5, 2024, a second paper summarizing the findings of this long-term study was released [4]. It concentrated on the ability of coronary artery calcium (CAC) scoring to predict major adverse cardiovascular events (MACE) in patients with stable chest pain.
Importantly, all participants were initially referred for invasive coronary angiography (ICA). The study specifically focused on this ICA-referred group and patients with stable chest pain (a moderate chance of blocked arteries). This perspective may offer valuable information for doctors deciding whether to perform ICA on such patients. What are the results?
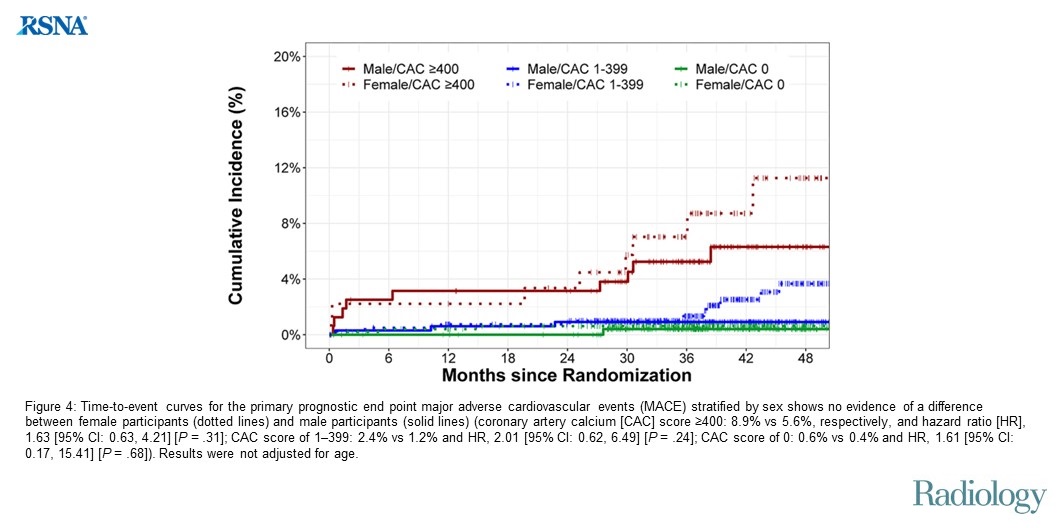
Image source: Biavati F. Published Online: March 05, 2024 https://doi.org/10.1148/radiol.231557
Calcium Score’s role in patient management strategies
The DISCHARGE study found a clear link between the severity of coronary artery calcification and patient outcomes. The percentage of people with confirmed coronary artery disease jumped significantly from 4.1% in those with a CAC score of 0 to 76.1% in those with a score of 400 or higher. Similarly, the need for procedures to open blocked arteries (revascularization rates) increased dramatically, from 1.7% to 46.2% across these groups. Patients with a CAC score of 0 or between 1 and 399 had a lower risk of major heart problems (MACE) compared to those with a score of 400 or higher (6.8%).
The study provides intriguing insights into patient management. If the risk of CAD development in patients with a low Calcium Score is relatively low, is it necessary to hospitalize them and send them for invasive diagnostics? And remember, this entire group was previously referred for such tests.
The knowledge that translates into money. Or not
Indeed, the study basically asks a question about financial efficiency and how to manage healthcare budgets. Interestingly, Prof. Dr. Marc Dewey – awarded with The Wilhelm Conrad Röntgen Prize in 2009 and the Marie Curie Ring in 2012 – started with these questions more than a decade ago [5].
We know and the DISCHARGE study also proved that a CT scan can accurately rule out CAD. It seems cost-effective to skip cardiac catheterization for low-risk patients. And we all love cost-effectiveness. But who would benefit from this cost saving?
At Graylight Imaging we’d like to focus on patients and society’s perspective. We should aim to find how much society can save by optimizing diagnosis. However, because of health budget policies, hospitals sometimes see things differently. Invasive procedures are financially incentivized by the system (higher reimbursement rates), leading to higher profits for them. It looks like a vicious cycle.

Is this the future now for everyone with chest pain?
Coronary artery calcification score based on CT scan can non-invasively identify symptomatic patients with stable chest pain. The low CAC score translates into a very low risk of heart attacks or strokes. Coronary artery calcium score is a great and cost-eff tool for risk stratification. However, there is still a “zero calcium paradox”, meaning artery calcification cannot be a singular predictive tool.
A recent paper in The Journal of the American College of Cardiology highlights this issue [6]. A zero CAC score does not necessarily guarantee clear arteries. A lack of calcification doesn’t mean there’s no plaque, because calcium scoring misses… non-calcified buildup.
Calcified and non-calcified build-up: developing possibilities
In the diagnosis of CAD, AI algorithms are emerging as valuable tools for the detection of both calcified and non-calcified atherosclerotic plaque. This allows for the identification of even subtle abnormalities, particularly non-calcified plaque which may be missed by traditional methods. Nowadays, coronary artery calcification score results are available to physicians within minutes. Quite a revolution has taken place in CAC scan scoring since Agatston and Janowitz’s first technique in 1990.
By improving risk stratification, AI has the potential to significantly impact society by reducing healthcare costs, minimizing unnecessary procedures… And saving lives.
References:
[2] Lin, CS., Liu, WT., Tsai, DJ. et al. AI-enabled electrocardiography alert intervention and all-cause mortality: a pragmatic randomized clinical trial. Nat Med (2024). https://doi.org/10.1038/s41591-024-02961-4
[3] DISCHARGE is a large research project involving multiple countries in Europe. It brings together 31 teams from 18 European nations. The project’s main focus is a practical study comparing different approaches, with 26 participating hospitals across 16 European countries. It aims to determine the best way to diagnose suspected coronary artery disease (CAD) in people with stable chest pain. https://www.dischargetrial.eu/
[4] https://pubs.rsna.org/doi/10.1148/radiol.231557
[5] https://healthcare-in-europe.com/en/news/roentgen-prize-for-marc-dewey.html